As well as feelings of fear and an inability to think straight, symptoms can include a pounding heart, dry mouth, excessive perspiration, insomnia, fatigue, headaches and muscle tension. Dealing with the normal challenges of daily life can be a trigger – walking into a room of people, getting stuck in traffic, travelling to an unfamiliar place, having to talk at a meeting, for example. But anxiety can also occur with no obvious cause, leaving sufferers feeling frustrated that they cannot control these reactions. However, as we’ll see, willpower alone is not the answer. Researchers working in the field of neuroscience have found that emotions operate at a much higher speed than thoughts and can frequently bypass the mind’s linear reasoning process entirely.1 The part of the brain involved in emotional processing – the amygdala – also evolved before the cognitive, ie thinking, part of the brain, and is highly attuned to potential danger, so is hyper sensitive to possible threats.
What this means in practice is that a past event, which at the time seemed threatening, can then set a pattern for future reactions. And because this trigger is often held in the subconscious, it can be hard to identify. So, for example, witnessing an angry exchange between your parents as a young child may then make you terrified of anger and confrontation. Also, if you experience a particularly challenging period that causes you to feel extreme stress or anxiety, your amygdala can become hyper-reactive, so will be looking for other potential triggers. This means you can find yourself in panic mode before your rational brain can evaluate a situation to see if such a response really is necessary. This state is referred to as ‘emotional hijacking’. One of the best approaches for dealing with this is HeartMath.
But there’s a lot you can do with your nutrition and lifestyle. While you are working towards adopting a consistently calmer way of being, steer clear of activities that significantly raise your heart rate, as these may confuse the brain into thinking you’re in an emergency situation. Opt instead for activities that help to relax and raise your natural energy levels like yoga, meditation or t’ai chi. Likewise, avoid stimulants that get your heart racing – coffee, tea, cigarettes, colas, energy drinks, chocolate and caffeine pills.
In pursuit of GABA: the antidote to anxiety
Most people, when faced with an intense or constant feeling of anxiety, will either ‘self-medicate’ with alcohol or cannabis, or see their doctor, possibly to be given a prescription for a tranquilliser, now called mood stabilisers. In one week in Britain, we pop something like 10 million tranquillisers, puff 10 million cannabis joints and drink 120 million alcoholic drinks.
The choice of these three drugs – alcohol, cannabis and tranquillisers – is no coincidence. They all promote the neurotransmitterA neurotransmitter is a chemical messenger that carries signals between body cells. They are various types of neurotransmitters which play a major role in everyday… GABA, which is the brain’s peacemaker, helping to turn off excess adrenalin and calm you down. That’s why that beer or glass of wine makes you feel sociable, relaxed, happy and less serious, at least for an hour as GABA levels rise. But after an hour or so GABA starts to fall and you feel irritable and disconnected, so you have another one, and another one. The trouble is that after a session of drinking, GABA levels become very suppressed, leaving you grumpy and irritable. So most of us avoid this by drinking in the evening and going to sleep under the influence. What we don’t realise is that alcohol also disturbs the normal cycle of dreaming, and it’s dreaming that regenerates the mind. So, when you wake up in the morning, you’re mentally tired, grumpy and irritable because of the low GABA, dehydrated, and feeling sluggish as your body detoxifies the alcohol from the night before. The net effect is that alcohol, in the long run, makes you more anxious, not less. The same is true for cannabis, which, if habitually smoked, also reduces drive and motivation.
1.5 million people in Britain are addicted to tranquillisers
The most common anti-anxiety drug is the benzodiazepine family of tranquillisers, such as Valium (diazepam), Librium and Ativan. These are highly effective at reducing anxiety in the short term, but highly addictive in as little as four weeks. For this reason doctors are strongly advised not to prescribe these for more than four weeks. Despite this, a poll carried out by Panorama found that 3 per cent of people questioned, equivalent to one and a half million people nationally, have been on tranquillisers for more than four months. Of these, 28 per cent had been on them for more than 10 years. A report by the National Addiction Centre, Kings College London, for prescriptions up to 2009, also found that a third of prescriptions were for more than eight weeks.2
These highly addictive drugs are now less likely to be prescribed, and have been replaced by newer, more profitable non-benzodiazepines such as benzodiazepines such as zolpidem, espopiclone and zaleplon on the apparent basis that they are safer.
However, even leaving the addictive nature of these drugs aside, a recent study in the British Medical Journal reports that patients prescribed zolpidem, temazepam and other hypnotics for reducing anxiety and aiding sleep suffered four times the mortality compared to matched patients not prescribed hypnotics.3 “Even patients prescribed fewer than 18 hypnotic doses per year experienced increased mortality, with greater mortality associated with greater dosage prescribed,” reports the author Dr Scripps, an expert in insomnia from California. There was also a 35 per cent overall increase in incidence of cancer among those prescribed high doses.
The sad truth is that tranquillisers, much like alcohol, increase anxiety and depression in the long run, as well as being addictive. With tranquillisers, however, the reason is slightly different. Tranquillisers open up the brain’s receptor sites for GABA, making the brain more sensitive to its effects. So you feel more relaxed, less anxious. The next day, however, you can feel ‘hung over’. The more often you take them, the more you need to get the same effect and, without them, you can get rebound anxiety and insomnia. Luckily, there is an alternative.
How to unwind with natural relaxants
States of anxiety are associated with too much of the stress hormones adrenalin and cortisolCortisol has been nicknamed ‘the stress hormone’ as it is released in higher levels during the body’s flight or fight response to stress. Levels of…, as shown in the diagram below. This is fuelled, not only by stressful thoughts, but also by caffeine and blood sugar dips, which stimulate the release of adrenal hormones.
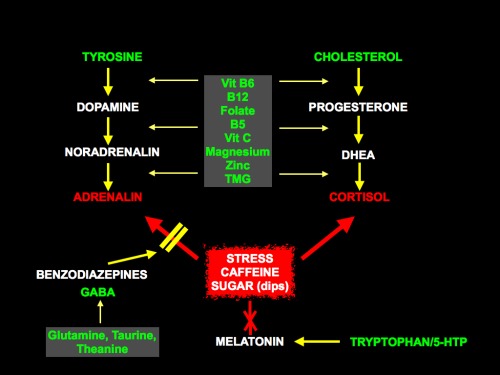
That’s why it is critical to quit stimulants and follow a low GL diet. Caffeine suppresses melatonin for up to 10 hours, thus stress and caffeine means poor sleep. Coffee is much worse than tea, the latter containing the relaxant theanine (see below). Green tea has the most theanine and least caffeine.
Some people need a little more extra help to learn how to switch out of the adrenalin state. There are breathing and meditation techniques for this. Reframing your approach to life can also be helpful. If you believe the root of your anxiety is embedded deep in your subconscious, there are also psychotherapeutic approaches that can help you to access and release negative programming, such as Emotional Freedom Technique (EFT), EMDR (Eye Movement Desensitization and Reprocessing), hypnotherapy and Time Line Therapy. These are worth checking out.
On the biochemical side, there are natural GABA promoters that ensure you produce and release GABA when you need to. These include amino acidsAmino acids are commonly known as the building blocks of protein. There are 20 standard amino acids from which almost all proteins are made. Nine…, minerals and herbs. A combination of all the nutrients shown in green in the diagram above is a great way to chill out. Tyrosine is not a relaxant as such, but helps if you have become adrenally exhausted.
GABA: the antidote to anxiety
GABA (gamma-amino-butyric acid) is the main inhibitory or calming neurotransmitter. It not only calms down excess adrenalin, noradrenalin and dopamineDopamine is a neurotransmitter (chemical messenger) found within the brain. It has a variety of influences on brain function including playing a role in regulating…, it also works together with serotoninSerotonin is a hormone found naturally in the brain and digestive tract. It is often referred to as the ‘happy hormone’ as it influences mood…. to keep you in a good mood. For these reasons, having enough GABA in your brain is associated with being relaxed and happy, while having too little is associated with anxiety, tension, depression and insomnia.4
GABA is not only a neurotransmitter, it’s also an amino acid. This means it’s a nutrient and, by supplementing it, you can help to promote normal healthy levels of GABA in the brain. There is one problem, however. In the European Union, GABA has been classified a medicine, meaning it is no longer available over the counter in the UK. You can buy GABA supplements on the Internet from countries such as the US, though. If you can get hold of GABA, supplement 500 to 1,000mg, once or twice a day as a highly effective natural relaxant. But note that while it is not addictive, that doesn’t mean there are no side-effects in large amounts. Up to 2g a day has no reported downside; however, if you go up to 10g a day, this can induce nausea or even vomiting, and a rise in blood pressure. So use GABA wisely, especially if you already have high blood pressure, starting with no more than 1g a day, and do not exceed 3g a day.
Taurine and Glutamine: GABA’s best friends
Taurine is another relaxing amino acid, similar in structure and effect to GABA. Many people think taurine is a stimulant because it is used in so- called ‘energy drinks’, but it is not. It helps you relax and unwind from high levels of adrenalin, much like GABA. Taurine has many other uses as well, including for insomnia, depression and even the ‘high’ phase of manic depression. Together with glutamine, the body can make more GABA. Try 500 to 1,000mg of taurine, twice daily together with the same amount of glutamine, for a natural GABA boost. There are no known cautions or adverse effects at reasonable doses. Some relaxing supplements provide this combination.
Valerian: nature’s valium
Another excellent anti-anxiety herb is valerian (Valeriana officinalis). Derived from the dried rhizomes and roots of an attractive perennial with pretty pink flowers, it grows throughout Europe in wet soils. As a natural relaxant it is useful for several disorders such as restlessness, nervousness, insomnia and hysteria, and it has also been used as a sedative for ‘nervous’ stomach. Valerian acts on the brain’s GABA receptors, enhancing their activity and thus offering a similar tranquillising action as the Valium-type drugs but without the same side-effects. As a relaxant you need 50 to 100mg twice a day, and twice this amount 45 minutes before retiring for a good night’s sleep. Since valerian potentiates sedative drugs, including muscle relaxants and antihistamines, don’t take it if you are on prescribed medication, without your doctor’s consent. Valerian can also interact with alcohol, as well as certain psychotropic drugs and narcotics.
Hops and passion flower: favourite of the Aztecs
Hops (Humulus lupulus) are an ancient remedy for a good night’s sleep and probably included in beer for that reason. Hops help to calm nerves by acting directly on the central nervous system, rather than affecting GABA receptors. You need about 200mg per day, but the effect is much less than valerian and most effective when taken in combination with this and other herbs such as passion flower. Passion flower (Passiflora incarnata) was a favourite of the Aztecs, who used it to make relaxing drinks. It has a mild sedative effect and promotes sleep much like hops, with no known side-effects at normal doses. Passion flower can also be helpful for hyperactive kids. You need around 100 to 200mg a day. Combinations of these herbs are particularly effective for relieving anxiety and can really help break the pattern of reacting stressfully to life’s challenges.
Magnesium: relaxing mind and muscle
MagnesiumWhat it does: Strengthens bones and teeth, promotes healthy muscles by helping them to relax, also important for PMS, important for heart muscles and nervous… is another important nutrient that helps you relax. It’s also commonly deficient. Magnesium not only relaxes your mind, it relaxes your muscles. Symptoms of deficiency therefore include muscle aches, cramps and spasms, as well as anxiety and insomnia. Low levels are commonly found in anxious people and supplementation can often help. You need about 500mg of magnesium a day. Seeds and nuts are rich in it, as are vegetables and fruit, but especially dark green leafy vegetables such as kale or spinach. I recommend eating these magnesium-rich foods every day and supplementing an additional 300mg. But, if you are especially anxious, and can’t sleep, supplement 500mg in the evening.
Theanine: why tea is better than coffee
In studies when caffeine levels are matched, the effects of tea and coffee on mood are very different5,6. This may be because tea also contains the natural amino acid l-theanine, a relaxant. Research suggests that 50mg L-theanine naturally stimulates activity in the brain, known as alpha waves, which are associated with a relaxed but alert mental state7,8. Supplements containing L-theanine and the amino acid GABA can help to make you feel more relaxed and less ‘edgy’.9 A trial of 400mg of theanine has been shown to help boys with ADHD get to sleep.10
Don’t panic – nothing is under control
Some people experience panic attacks, characterised by extreme feelings of fear. These are not at all uncommon. Symptoms often experienced during a panic attack include palpitations, rapid breathing, dizziness, unsteadiness and a feeling of impending death. Those who suffer with agoraphobia, a fear of being alone or in public places, often know that they can go out or can be alone, but are afraid of having a panic attack.
As ‘psychological’ as this sounds, there is a biochemical imbalance behind many people’s anxiety attacks, apart from, or as well as, any psychological factors. It’s too much lactic acid. When muscles don’t get enough oxygen, they make energy from glucose without it. The trouble is there’s a by-product called lactic acid. As strange as this might seem, giving lactic acid to those prone to anxiety attacks can induce an anxiety attack.11
One way to increase lactic acid levels is to hyperventilate. Many people will do this when they’re experiencing anxiety attacks. Hyperventilation changes the acid level of the blood by altering the balance of carbon dioxide. The body responds by producing more lactic acid. The solution is to breathe into a paper bag during a hyperventilation attack and concentrate on breathing deeply for a minute. This helps redress the balance. Moments of blood sugar dips can also both bring on hyperventilation and increase lactic acid. So, keep your blood sugar level even by eating little and often.
A more advanced and highly effective breathing technique is Buteyko breathing. It is good for general anxiety but especially good for those who often hyperventilate and have panic attacks, which can be exacerbated by the lack of CO2 induced by over-breathing. Buteyko breathing can be taught in a workshop or one-to-one session. See my Special Report on this.
The other main driver of panic attacks is just too much adrenalin. Many people don’t realise that the essential hormone progesteroneProgesterone is one of the main female sex hormones…. is anti-adrenalin. When levels fall low, commonly in the peri and post menopausal phases, women often become more anxious and prone to panic attacks. Simply rubbing natural (bio-identical) progesterone cream on the inner arms, where is absorbs well, can literally stop panic attacks in under five minutes. Dr Michael Platt has written a book about this, called Adrenalin Dominance, available from www.plattwellness.com. To read more about natural progesterone see my Special Report on Bioidentical Hormones.
An instant way to switch off anxiety
If you experience a panic attack or extreme anxiety, dipping your face into a basin of very cold water for 30 seconds (while holding your breath, of course) can instigate what’s called the Dive Reflex, which has a rapidly calming effect. This is because cold water stimulates your vagus nerve, which is a key part of your parasympathetic nervous system (PNS). The PNS works in partnership with your sympathetic nervous system (SNS), which is involved in the stress response. So after a stressful event has passed, it’s your PNS that takes over to calm you down and restore your body to business as usual. But triggering the Dive Reflex activates the PNS immediately, so you feel calmer and less stressed in a matter of seconds. Splashing your face with icy water, or pressing your face onto a plastic bag filled with ice, can also have the same effect for some people, and works better if you also lean forward and hold your breath for 30 seconds. The only word of caution is that this procedure should not be attempted by anyone with a slow heart rate or low blood pressure, as it slows your heart rate.
Case Study
Emily: “I recently started getting panic attacks after an unpleasant week of events in which the future life as I knew it became uncertain. On return to normality panic attacks begun. I was never sure what set them off but was in a constant state of shaky nerves, high heart rate, no appetite and feeling hot and sweaty for a month and I couldn’t work out why. I can happily say it’s now been a 3 week panic free period. I learnt about progesterone cream and the dive technique which both dramatically helped stop the panic attacks in the moment from a 12hr panic to nothing. Stopping the onset of them came from a trip away, I had time to breathe and get to know my non panicky self, with the knowledge that I could stop them at any time if they returned.”
Stress reduction techniques
Some people need a little extra help to learn how to switch out of the adrenalin state. There are breathing and meditation techniques for this, as well as psychotherapeutic avenues to explore in dealing with the perceived stresses and causes for anxiety, and many of them can be extremely helpful. I have been particularly impressed by Heart Math techniques and also the effects of ‘vital energy’ exercises such as yoga, T’ai chi and also Psychocalisthenics.
Supplement Glycine
Another approach that works for many is supplementing glycine during a panic attack. Glycine switches off noradrenalin thus reducing the feeling of panic. The best way to get it in fast is to break open four capsules (usually 500mg) putting 2 grams under your tongue where it can absorb sublingually more quickly than orally. You can keep doing this every few minutes, up to a maximum of 10 grams. No side-effects have been reported at these doses.
Finally, deficiency in vitamin B1 stops the body breaking down glucose properly, again promoting lactic acid. So, make sure you are supplementing a good B complex or multivitamin. Also, check yourself out for food allergies. These are the most common biochemical imbalances that can lead to panic attacks.
An integrated approach works best
While the causes for high levels of anxiety are often psychological, by balancing blood sugar, reducing stimulants, ensuring optimum nutrition, plus judicially using these natural anti-anxiety herbs and nutrients, you can break the habit of reacting with fear and anxiety to life’s inevitable stresses. Addressing the potential underlying triggers for anxiety is also important.
In terms of supplements, often, a combination of relaxing amino acids and herbs is the most effective for reducing high levels of anxiety. The synergistic action of nutrients and herbs such as GABA or taurine plus glutamine, valerian, hops and passion flower, magnesium and 5-HTP also means the doses for each can be lower. These are my favourite ‘chill’ food ingredients, taken in the evening, or an hour before bed. If you are also exhausted and unable to cope with stress, try an ‘awake’ formula containing tyrosine, plus adaptogenic herbs in the morning. Two of these before breakfast, and two chill supplements in the evening, for one month, is a great support to get yourself back on track.
- LeDoux JE, The Emotional Brain: The Mysterious Underpinnings of Emotional Life, 1996
- NOP Poll, May 2001, Panorama, BBC, UK
- Shiahm IS and Yatham N, Life Sciences, 1998
- Hindmarch I et al, Psychopharmacology, 1998
- Hindmarch I et al, Psychopharmacology, 2000
- Juneja LR, et al, Trends Food Sci Tech, 1999
- Nobre AC et al., a report to Unilever by the Department of Experimental Psychology, University of Oxford, 2003
- Unno K et al, Pharmacol Biochem Behav, 2013
- Lyon et al, Altern Med Rev, 2011
- Pitts FN and McClure JN, New Engl J Med, 1967
- Rakhimov A, Normal Breathing – The key to Vital Health; see also Fried R, The Hyperventilation Syndrome

Comments
Join the Conversation on our Facebook Page