Mismatched molecules
“Replacing the oestrogenOestrogen is one of the main female sex hormones…. that your body is no longer producing with the versions found in conventional HRT is like replacing parts designed for a Chevvy with those made for a Mercedes,” says Dr Jonathan Wright, Medical Director of Tahoma Clinic in Washington USA, and a long-time advocate of what are known as bio-identical hormones. “They may be roughly the same, but with both engine parts and biology, very precise measurements matter.”
The idea of bio-identical hormones has been attracting a lot of attention in America, especially since actress Suzanne Somers, previously best known for her role as a ditzy blonde in the 1980s sitcom hit Three’s Company, published a best-seller on their benefits.(3) However claims that they are safer or more effective has been dismissed as “marketing” by the American drugs authority, the FDA.
Here in the UK, the situation is typically much more low-key. There’s been far less publicity about them, although a small but growing number of women have been taking them. Several brands are available on the NHS, however most GPs are reluctant to prescribe them, saying there is no evidence they work. So what exactly does it mean to say that a hormone is bio-identical? A regular HRT pill contains oestrogen – the hormone that promotes growth so it’s good for skin and hair, lifts depression, controls hot flashes – along with progesteroneProgesterone is one of the main female sex hormones…., the hormone that’s produced to prepare your body for pregnancy.
Not all oestrogens are equal
Just to complicate matters oestrogen in the body comes in three varieties – oestrodial, oestrone and oestriol. Not only that but they come in very different proportions. Oestriol is the weakest and pre-menopausal women normally have lots of it; it makes up about 90 per cent of the total amount. The next most abundant is oestradiol, the most potent one, at around 7 per cent, followed by oestrone at 3 per cent. But in regular HRT, the oestrogen part doesn’t come in anything like those proportions. One of the most common brands is one called Premarin which actually comes from the urine of pregnant mares. Not only are the proportions very different but it also contains extra horse oestrogens. Oestrone shoots up from being the least to the most abundant at 75 per cent; next comes oestradiol which, together with two other horse oestrogens, makes up between 6 and 15 per cent. And finally you get 5 to 19 per cent of another horse hormone called equilin. Very different. Even in hormones which are molecularly very similar, the difference in effect can be huge. One way of summing up the difference between men and women would be that it is the difference between early exposure to testosteroneTestosterone is a male sex hormone important for sexual and reproductive development…. or oestrogen. But as these below pictures show, the oestrogen oestrodial is actually more like testosterone than it is like Premarin. Yet women are advised that premarin is a suitable replacement for oestrogen. 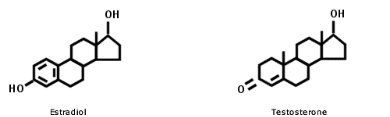 Why progesterone is key
Why progesterone is key
The other hormone that’s found in regular HRT is called a progestagen, or sometimes a progestin. These are non-identical versions of the hormone progesterone. During menopause the amount of progesterone in your body drops more dramatically than oestrogen, to almost zero. Non-identical progestin is added to regular HRT to reduce the risk of womb cancer which is raised by giving oestrogen on its own. You can get an idea of how big the difference is between bio-identical progesterone and progestin from their effect on pregnancy. Progesterone is the hormone that the body makes to support pregnancy – it’s used as part of infertility treatments – while progestin raises the risk of congenital abnormalities and miscarriage. According to NHS Direct, other progestin side effects include breast tenderness, headaches, mood-swings and depression. The main side-effect of progesterone is sleepiness.
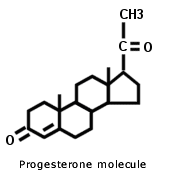
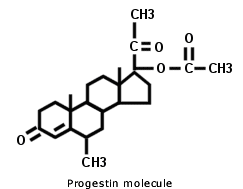 Examining the evidence
Examining the evidence
So are the identical versions of these hormones safer and more effective? It’s an attractive idea that makes sense but what’s the evidence? At the moment if you want it proved in a big trial comparing the two, then it’s not there. But there are plenty of people who find that, quite apart from the possible long-term risks of regular HRT, that it just doesn’t agree with them, while a switch to bio-identical HRT (BHRT) transforms them.
“Starting the menopause was hell,” says Sharon, an advertising executive with two teenage children and a husband who, she admits, was losing patience with her wild mood swings. “My GP suggested anti-depressants, but I knew I wasn’t depressed. I just wasn’t myself any more.” It was then that Sharon heard about Dr Gluck. “The first thing she did was to listen to me. I felt that everyone else was trying to offer me a ready-made solution. She then did something else that oddly no one else had done, which was to measure what my hormone levels actually were. “It turned out that my oestrogen level wasn’t too bad but that I had almost no progesterone, so my oestrogen wasn’t being balanced. She explained that progesterone affects a brain chemical called GABA, which is targeted by tranquilisers, which is why it has a calming effect.” Sharon was given a progesterone cream to rub in and within six weeks, the mood swings had gone and she was functioning normally again. Apart from using bio-identical hormones which, she says, are gentler and better tolerated, Dr Gluck also treats the individual patient rather than offering a similar combination to every one. “Some need more oestrogen or progesterone but I check other hormones like testosterone which is vital for a woman’s sex drive, and thyroid, low levels of which can result in fatigue and depression.” But this approach gets very little support from most NHS GPs, who may point to a few small studies that have found no benefit from using progesterone.
The official advice is that providing you have as low as possible a dose of regular HRT and don’t stay on it for any longer than five years, your risks of any problems are very low. “There is absolutely no evidence that bio-identical hormones are any safer,” declares Dr Sarah Jarvis, speaking for the Royal College of GPs. But the official view of the Royal College would be thought curious in France, where both progestins and progesterone are widely used. Because of this, there is much more research done on the difference between them. Here in the UK, progestins are only included in HRT to stop cancer developing in the lining of the womb. But French studies suggest that progesterone has all sorts of other benefits, almost none of which come from progestins.
Lessons from France
“There is evidence that progesterone has beneficial effects on the breast tissue, on blood vessels and for strengthening bones,” says Dr Michael Schumacher of the Kremlin-Bicêtre hospital in Paris, “although more research needs to be done. Many of the benefits of progesterone comes from the fact that while oestrogen stimulates cells, progesterone calms them down.”(4) As a result, one striking claim for progesterone is that it might lower your risk for dementia.
In the brain, oestrogen and progesterone combine to protect cells, while progestins reduce this protective effect. “There is strong evidence that the ageing nervous system remains at least to some extent sensitive to the beneficial effects of progesterone,” says Schumacher. While the Women’s Health Initiative (WHI) study showed that combining progestins with oestrogen slightly raised the risk of strokes and breast cancer, Schumacher’s work explains how progesterone can lower these dangers. “Oestrogen combined with progesterone could make for a safe and effective form of HRT,” he says. “Although such an option may not be very attractive for the pharmaceutical industry.” The reason for this is that progesterone is not patentable, precisely because it is a natural substance, and so it won’t be a big money spinner. The claim that progesterone may protect against breast cancer is backed up by a big ongoing French study of 54,548 menopausal women, comparing what happens to those who take progesterone in their HRT with those who get progestin.
The latest report has found that after eight years, while those on progestins have a raised risk of breast cancer, those on progesterone don’t.(5) As a result of this research there has been a change in prescribing in France. “After the WHI study, many women had stopped taking oestrogen pills,” says Dr Virginie Ringa of the French Institute for Health and Medical Research, Le Kremlin-Bicêtre, Paris. “Now they are taking an oestrogen patch together with progesterone which is taken orally. But it is true that none of this has been tested in large clinical trials.”
Can progesterone reduce stroke risk?
Meanwhile in America, Dr Schumacher’s claim that progesterone can protect blood vessels and cut down the risk of strokes has just been supported in two small trials at Texas University. Researchers gave a progesterone cream or a placebo to 30 post-menopausal women for eight weeks. Not only did the cream improve their symptoms but there was no rise in various markers in the blood that make strokes more likely, such as inflammation and a tendency to form clots.(6) “We also found similar beneficial results when we gave a cocktail of individualised bio-identical hormones to 75 patients and compared the results to regular HRT,” says Dr Kenna Stephenson, Assistant Professor of Family Medicine at The University of Texas Health Center. The women were tested after a year. The results were reported at the American Heart Association annual meeting in November 2008.(7) “Last year the FDA issued an alert on the dangers of bioidentical hormones, yet our 12 month data would suggest that they are safe and effective for peri/post-menopausal women when high quality creams are used,” says Stephenson.
Call for more research
Now evidence like this doesn’t completely prove the case for bio-identical hormones and everyone agrees there needs to be more research. So will the big trials that doctors are demanding now be run? The depressing truth is that it’s unlikely without strong consumer pressure. Calls for such research are not new. Thirty years ago an editorial in the Journal of the American Medical Association asked how long clinicians will have to wait for proper clinical trials on the benefits of oestriol, the weakest of the oestrogens. “Enough evidence has been accumulated,” it said “that we may say that it is safer than oestrone and oestradiol.” The trials have still not been done.(8)
What to do if HRT is not working for you
If you are unwilling to wait and HRT isn’t working for you, what can you do? You can go to a private doctor who specialises in hormones, like Dr Gluck, As well as prescribing bio-identicals, these practitioners will check the state of your hormones in general using a salivary hormone test. Dr John Moran, who also works in London, explains that this is useful because the level of one hormone can affect the working of another. “Oestrogen, for instance, needs to be balanced by testosterone or you are likely to see an increase in inflammation,” he says. “Low levels of progesterone may affect thyroid function.” Another fan of bio-identical hormones is Dr Shirley Bond, who I interviewed in the May 2006 newsletter. In most cases, she finds there is both a deficiency in oestrogen and oestrogen dominance (meaning very low progesterone).
Since the body can make oestrogen from progesterone if it needs to, her first option is to use a transdermal progesterone cream. “I start with a 3 per cent progesterone cream, giving a dollop (the equivalent of 20 to 40mg) per day in the second half of the menstrual cycle,” she says. “If there’s no menstrual cycle, then I recommend three weeks on progesterone and one week off. Hormone expert Dr John Lee (author of What Your Doctor Didn’t Tell You About The Menopause) used to say that progesterone was good for sweats and hot flushes. I don’t find that it always works. Some women do better with a combination of progesterone and isoflavonesIsoflavones are naturally occurring compounds – many act as phyto-oestrogens. An example of an isoflavone is Soya Isoflavones…. – a red clover supplement, for example.” “If that doesn’t do the trick, then I give Uterogestan, which is a progesterone pill, combined with Hormonin. Hormonin is a combination of oestradiol, oestrone and oestriol, which are the three types of oestrogen that a woman’s body produces. This is much more sophisticated and safer than giving just oestradiol. As soon as it starts working, I reduce the oestrogen dose to half a Hormonin tablet per day, or even a quarter-tablet per day. In fact, I like to get the dose as low as possible. “When the oestrogen dose is low enough, I switch from the progesterone pill to a cream (which provides less progesterone). Occasionally, I’ll add the herb black cohosh in combination with Phytosoya vaginal gel (made by Arkopharma).”
Topping up testosterone
One of the most common complaints of peri and menopausal women is a loss of sex drive. After the menopause, sex can become more painful due to vaginal dryness and thinning of the vaginal mucosa. Dr Bond recommends a soya-based gel. Recent animal research confirms that this does have an effect.9 (9) “If that doesn’t work, I recommend Ovestin, which is an oestriol cream,” she says. “This is a gentler form of oestrogen than oestradiol, and I always advise using it in conjunction with progesterone cream.” Testosterone deficiency is a common cause of lack of sex drive, in both men and women, the only difference being that men tend to make and need more of it. It’s a hot topic in the medical journals. Two recent studies have found benefit with greater effect at higher doses, although that has to be balanced by greater risk of unwanted hair growth.(10) (11) Dr Bond and Dr Gluck often recommend testosterone for women. “I think it can be very important, especially for women who have lost their sex drive. It can help with libido,” says Bond. “I may recommend Testogel, a transdermal testosterone cream designed for men, but women should use less than the full dose. I don’t like testosterone implants. They often deliver too much testosterone, which can make women too aggressive.”
What’s available on the NHS
If regular visits to a private doctor are not a financial option, then bio-identical hormones are available on the NHS, so ask your doctor about them. The oral progesterone used in France – called Utrogestan here – is now licensed in the UK for treating the menopause. And so are patches or creams containing bio-identical oestrodial, which is then absorbed directly through the skin; brands include Estrogel and Estraderm. Hormonin will give you the three oestrogens in a bio-identical form. Doctors can also prescribe Pro-juven, a transdermal progesterone cream, as an unlicensed medicine. It seems the critical issue is getting tested and then applying the right balance of bio-identical hormones in amounts equivalent to what your body would produce normally.
Useful information sources
• Natural Progesterone Advisory Network [www.natural-progesterone-advisory-network.com], an Australia-based information site.
• Natural Progesterone Information Service [www.npis.info] in the UK.
• Natural Menopause Advice Service [http://www.nmas.org.uk/about.htm], again based in the UK.
Also read:
• The Hormone Solution, Dr Thierry Hertoge, Three Rivers Press
References
1. Million Women Study Collaborators, Breast cancer and hormone-replacement therapy in the Million Women Study, British Medical Journal (2003), vol 362, no 9382.
2. RT Chlebowski et al (WHI Investigators), Breast cancer after use of estrogen plus progestin in postmenopausal women, New England Journal of Medicine (2009), vol 360 (6), pp 573-87.
3. S Somers, Ageless: The Naked Truth About Bioidentical Hormones (2006), Crown Publishing Group. ISBN 0-307-23724-9.
4. M Schumacher, R Guennoun, A Ghoumari et al, Novel perspectives for progesterone in HRT, with special reference to the nervous system, Endocrine Reviews (2007), vol 28 (4), pp 387-439.
5. A Fournier et al, Unequal risks for breast cancer associated with different hormone replacement therapies: results from the (E.sib.3) cohort study, Breast Cancer Research & Treatment (2008), vol 107 (1), pp 103-11.
6. K Stephenson, P Neuenschwander et al, Transdermal progesterone: Effects on menopausal symptoms and on thrombotic, anticoagulant and inflammatory factors in post menopausal women, International Journal of Pharmaceutical Compounding (2008), vol 12 (4).
7. K Stephenson, American Heart Association Scientific Sessions, New Orleans, 8-12 November 2008.
8. A Follingstad, Estriol the forgotten hormone? Journal of American Medical Association (1978), vol 239, pp 29-30.
9. TF Lien et al, Supplementary health benefits of soy aglycons of isoflavone by improvement of serum biochemical attributes, enhancement of liver antioxidative capacities and protection of vaginal epithelium of ovariectomized rats, Nutrition & MetabolismMetabolism is a term that is used to describe the chemical reactions that take place within the body’s cells. The body gets the energy it… (2009), http://www.nutritionandmetabolism.com
10. H Maia Jr, J Casoy & J Valente J, Testosterone replacement therapy in the climacteric: benefits beyond sexuality, Gynecological Endocrinology (2009), vol 25 (1), pp 12-20.
11. SR Davis, M Moreau, R Kroll R et al, Testosterone for low libido in postmenopausal women not taking estrogen, New England Journal of Medicine (2008), vol 359 (19), pp 2005-17.

Comments
Join the Conversation on our Facebook Page